Referral Management Best Practices: A Data-Driven Playbook for Healthcare Organizations
Most articles about referral management best practices offer the same generic advice: communicate clearly with specialists, follow up with patients promptly, track your referrals. That guidance is technically correct and practically useless. What you actually need are specific benchmarks to measure against, proven workflows you can implement, and a clear understanding of what separates high-performing referral operations from average ones.
Loading audio...
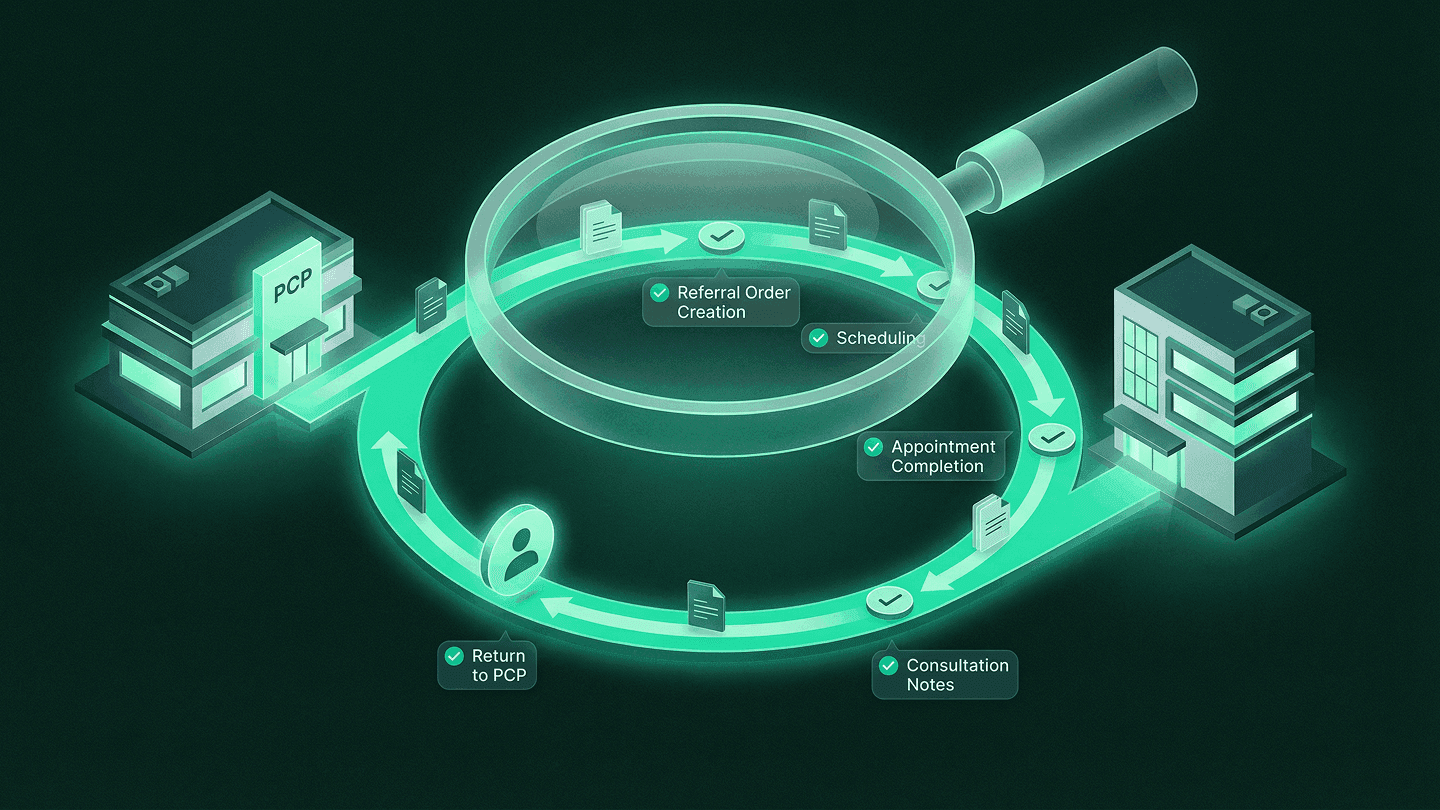
Featured Image: Data-Driven Referral Management Best Practices with KPI Benchmarks
Most articles about referral management best practices offer the same generic advice: communicate clearly with specialists, follow up with patients promptly, track your referrals. That guidance is technically correct and practically useless, like telling a drowning person to swim. The people searching for referral management best practices already know they should follow up with patients. What they need are specific benchmarks to measure against, proven workflows they can implement, and a clear understanding of what separates high-performing referral operations from average ones.
Having built and operated healthcare organizations that depended on referral coordination across 50 states, and now running Linear Health where we automate referral workflows for specialty practices and health centers, I've had the opportunity to observe what high performers actually do differently. The difference isn't a single magic practice. It's a systematic approach that combines measurement, process design, technology, and continuous improvement.
This playbook provides the specific benchmarks, workflows, and operational practices that drive referral performance, organized so you can identify where your organization has the most room for improvement and act accordingly.
The Benchmarks: What Good Looks Like
You can't improve what you don't measure, and you can't measure meaningfully without knowing what "good" looks like. These benchmarks come from published research, industry data, and what we observe across practices using our platform.
| Metric | Industry Average | Best Practice Target |
|---|---|---|
| Referral completion rate | ~50% | 85-95% |
| Time to first patient contact | 3+ days | Under 24 hours |
| Time to scheduled appointment | 10+ days | Under 5 business days |
| No-show rate | 20-30% | 12-18% |
| Closed-loop rate | Below 30% | Above 70% |
| PA first-pass approval rate | Below 80% | Above 90% |
Referral completion rate (patient seen by specialist): Industry average sits around 50%. Well-managed practices achieve 75-85%. Practices with automated multi-channel outreach and systematic follow-up reach 85-95%. If your completion rate is below 60%, you're in the bottom quartile and the opportunity for improvement is substantial.
Time from referral creation to first patient contact: Best practice is under 24 hours. Data shows that contacting patients within half a day yields an 84% scheduling rate. By day 3-5, scheduling rates drop to 50-60%. By day 7+, you've lost a significant share of patients who would have scheduled with faster outreach. If your average first contact is 3+ days, this is likely your single highest-impact improvement area.
No-show rate for specialist appointments: Industry average runs 20-30% for medical specialties, higher for behavioral health. Best practice for practices with smart reminder sequences is 12-18%. Practices achieving below 15% typically use multi-channel reminders (SMS + email + voice) at 7, 3, and 1 day before the appointment with same-day confirmation.
Closed-loop rate (consultation notes received by referring provider): Average is below 30%. Denver Health improved from 18% to 73.3% with systematic tracking. Target: above 70% as an intermediate goal, above 85% as a mature benchmark.
Best Practice 1: Speed Wins Everything
The single most impactful referral management practice is compressing the time between referral creation and patient contact. Everything else — scheduling efficiency, no-show prevention, closed-loop tracking — depends on getting to the patient while they're still engaged.
The psychological mechanism is straightforward. When a patient sits in their doctor's office and hears "I'd like to refer you to a specialist," their motivation to follow through is at its peak. That motivation decays rapidly. By the time your coordinator calls three days later, the patient may have rationalized that they don't really need to see a specialist, may have gotten busy with work and family, or may have simply forgotten.
Automated outreach within minutes of referral creation captures patients at peak motivation. An SMS message — "Hi [name], Dr. [referring provider] has referred you to [specialist] at [practice]. You can schedule your appointment here: [self-scheduling link]" — sent within 5 minutes of the referral order being created reaches the patient while they're still thinking about it, often while they're still in their car leaving the doctor's office.
At practices using Linear Health, this speed of outreach is automated. The platform detects the new referral in the EHR and triggers the outreach sequence without any coordinator intervention. For practices without automation, the actionable version of this best practice is establishing a "same-day contact" standard: every new referral receives first patient contact on the day it's created.
See how automation handles patient outreach
Linear Health contacts patients via SMS, voice AI, and email, converting 80% of referrals to booked appointments automatically.
Best Practice 2: Multi-Channel Persistence
One phone call to a patient who doesn't answer isn't outreach. It's a check-the-box activity. Effective referral outreach persists across channels and over time until the patient either schedules or is definitively flagged for coordinator follow-up.
A proven outreach sequence for inbound specialty referrals:
| Day | Channel | Action |
|---|---|---|
| Day 0 | SMS | Self-scheduling link (within minutes of referral) |
| Day 1 | Scheduling info + practice details (if no SMS response) | |
| Day 3 | SMS | Second message with different angle |
| Day 5 | Voice | AI voice or live phone call |
| Day 10 | SMS | Final message (referral will need re-initiation) |
| Day 14 | Escalation | Flag for coordinator review; notify referring provider |
This sequence accomplishes two things. First, it reaches patients through whatever channel they actually use. Some respond to SMS immediately, others need a phone call, others prefer email. Second, it creates multiple touchpoints over time, catching patients who weren't ready to schedule on day 0 but may be on day 5.
Best Practice 3: Standardize Documentation Before It's Needed
Prior authorization denials and referral processing delays frequently trace back to incomplete documentation. The specialist's office receives a referral with a diagnosis code and a patient name but no clinical notes, no imaging results, no relevant lab work. They can't schedule appropriately without this information, so they request it, adding days to the process and requiring coordinator time on both sides.
The best practice is standardizing referral documentation at the point of creation: define the minimum documentation set for each referral type (diagnosis, relevant clinical notes, recent imaging/lab results, insurance information, patient contact details) and build it into the referral order workflow so the documentation is collected before the referral is submitted.
For practices on Athena Health and similar EHR platforms, this can be configured through referral order templates that require specific fields before submission. For practices with more flexible workflows, a simple referral checklist that coordinators verify before transmitting the referral achieves the same result.
Best Practice 4: Treat Specialist Relationships Like Partnerships
High-performing referral operations don't just send referrals to specialists. They actively manage the specialist relationship to optimize patient outcomes and operational efficiency.
This means several specific practices:
- Designate 3-5 preferred specialists per specialty based on performance data (scheduling speed, communication responsiveness, patient satisfaction).
- Send consistent, well-documented referrals to preferred specialists, building volume that makes your practice a valued referral source.
- Establish communication expectations with specialist practices: when you'll send referrals, what documentation you'll include, how quickly they should contact patients, and how consultation notes should be returned.
- Track specialist performance quarterly and adjust preferred specialist lists based on data.
One health system that implemented this approach saw referrals to preferred in-network specialists increase from 30% to 62%, improving both patient experience (shorter wait times, better coordinated care) and network economics (retained downstream revenue).
Best Practice 5: Build Workflows by Organization Type
Referral management best practices aren't one-size-fits-all. The optimal workflow differs significantly by organization type.
For specialty practices (inbound referrals): Prioritize referral intake speed (fax parsing, chart creation), patient outreach speed and persistence, self-scheduling capability, no-show prevention, and referring provider communication. Your goal is converting every received referral into a completed appointment as quickly as possible.
For primary care groups (outbound referrals): Prioritize prior authorization automation, specialist matching and routing, patient engagement through the referral journey, completion tracking, and care gap reporting for value-based contracts. Your goal is ensuring patients complete specialist visits and that results inform ongoing primary care.
For FQHCs: Prioritize multi-language outreach, Medicaid MCO authorization management, UDS quality reporting integration, multi-site coordination, and patient engagement strategies that account for social determinants barriers. Your patient population faces unique access challenges that standard workflows don't address.
Best Practice 6: Measure, Report, and Improve Continuously
Implementing best practices without measurement produces temporary improvement that erodes over time as attention shifts to other priorities. Sustainable referral management requires ongoing measurement and regular review.
Weekly: Review the list of referrals that have stalled (not progressed to the next status within expected timeframes) and intervene. This is the operational heartbeat of referral management.
Monthly: Report on the core metrics (completion rate, time-to-scheduling, no-show rate, closed-loop rate, authorization first-pass rate) and compare to benchmarks. Identify trends and investigate any metrics that are declining.
Quarterly: Review specialist performance data and adjust preferred specialist lists. Evaluate whether workflow changes or technology investments are needed to address persistent bottlenecks. Review coordinator workload to ensure automation is handling routine work and human effort is focused on exceptions.
The practices that sustain high referral performance over time treat these reviews with the same discipline they apply to financial reporting or clinical quality reviews. Referral management is a revenue function and a care quality function. It deserves operational rigor.
Putting It All Together
The gap between average and excellent referral management isn't about knowing the best practices. It's about implementing them systematically and sustaining them over time. Speed of outreach, multi-channel persistence, standardized documentation, specialist relationship management, organization-specific workflows, and continuous measurement form a cohesive operating model that compounds improvement over time.
For practices looking to accelerate this improvement, automation platforms like Linear Health implement many of these best practices by default — automated same-day outreach, multi-channel persistence sequences, standardized referral documentation, closed-loop tracking, and real-time analytics. The technology handles the execution of best practices at scale while your team provides the clinical judgment and relationship management that no technology can replace.
The best time to start improving referral management was years ago. The second best time is this month, with clear benchmarks, a specific workflow, and the discipline to measure results.
Frequently Asked Questions About Referral Management Best Practices
What are the most important referral management best practices?
The six most impactful referral management best practices are: contact patients within 24 hours of referral creation (speed of initial contact is the strongest predictor of completion), use multi-channel outreach across SMS, email, and phone (practices using three or more channels achieve 85%+ completion), standardize referral documentation with complete clinical and insurance information, build structured specialist relationships with defined communication protocols, implement closed-loop tracking from referral to completion, and measure performance weekly against specific KPI benchmarks.
What referral completion rate should my practice target?
Practices should target referral completion rates above 80% as an operational benchmark. The industry average ranges from 50-65% depending on specialty and organization type. Top-performing organizations using automated referral coordination consistently achieve 85-95% completion rates. A 15-point improvement in completion rate for a practice processing 400 referrals monthly at $500 average revenue per visit represents approximately $360,000 in additional annual revenue.
How often should practices review referral management performance?
Practices should review referral management performance on three cadences: weekly for operational metrics (referral volume, completion rate, time to first contact, outstanding referrals requiring attention), monthly for trend analysis (completion rate trends, coordinator productivity, specialist performance, payer-specific bottlenecks), and quarterly for strategic review (specialist network optimization, workflow adjustments, technology investments, and staffing alignment). Treat referral reviews with the same discipline applied to financial and clinical quality reporting.
Ready to implement these referral management best practices at scale?
Book a 30-minute ROI assessment to see how automation delivers these best practices for your specific workflow.
Book ROI Assessment
Sami scaled Simple Online Healthcare to $150M and built a multi-specialty telehealth clinic across 20 specialties and all 50 states. Connect on LinkedIn.