Referral Coordination: What It Is, How It Works, and Why the Job Is Getting Harder
Referral coordination is the end-to-end process of getting a patient from a referral order to a completed specialist visit, with the loop closed back to the referring team. It's a defined operational function, not just a job title, and in most practices it's the point where care continuity is most likely to break.
Loading audio...

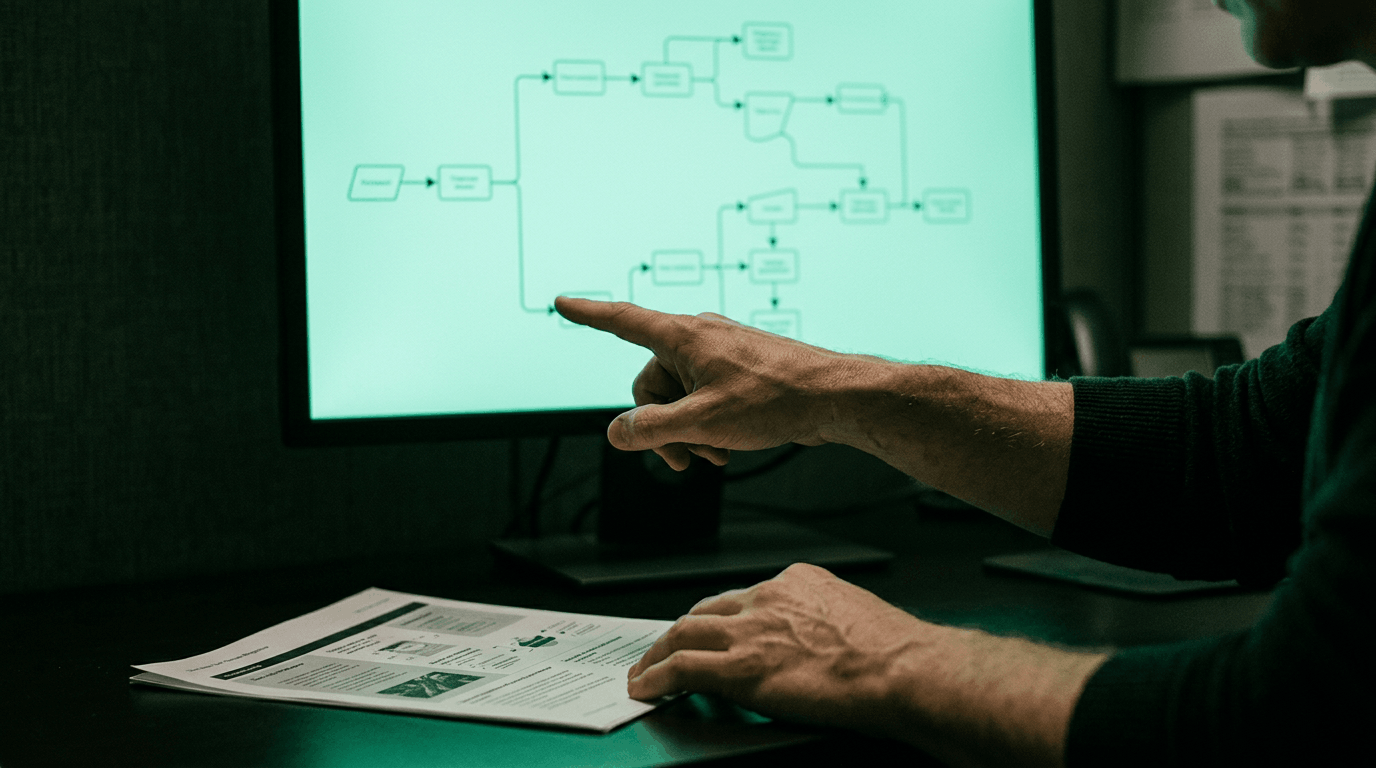
Featured Image: Referral Coordination as a Closed-Loop Operational Workflow
Referral coordination is the process of managing patient referrals end to end: initiating the referral, transferring clinical documentation, obtaining prior authorization, scheduling with the receiving provider, confirming patient follow-through, and closing the loop with outcome information. It is a defined operational function, not simply a job title.
The Agency for Healthcare Research and Quality defines care coordination as "deliberately organizing patient care activities and sharing information among all participants concerned with a patient's care." Referral coordination is that definition applied specifically to the handoff between providers, and in most practices it is the point where care continuity is most likely to break.
A referral coordinator is usually the person responsible for executing this process. But the process itself exists whether or not a single person owns it, and that distinction matters. When referral coordination is treated as a task rather than a workflow, steps fall through the cracks, patients don't show up, and neither the referring nor the receiving provider knows why.
This post covers what referral coordination actually means, how the workflow runs in practice, what skills and qualifications the role requires, what it pays (including state-level data for Florida), and what strong coordination looks like when it's working well.
The short version of where things stand: the referral coordination function has grown more complex faster than most practices have adapted their processes or staffing to match. The job is harder than it looks from the outside, and the consequences of getting it wrong are real.
What Does Referral Coordination Mean in Practice?
Most people think a referral is complete when the referring provider sends a fax or places an order. It isn't. A referral is complete when the patient is seen, the visit is documented, and relevant clinical information flows back to the referring team. Everything in between is referral coordination.
CMS guidance on referral workflows is clear that effective referral management requires "partners to work in coordination to optimize the outcome," with defined roles, mapped processes, and explicit clarity about whether a provider is co-managing the patient or transferring care entirely. That level of process definition is rare in most ambulatory settings.
The Closed-Loop Referral Workflow
A well-run referral coordination process follows six stages:
- Referral creation. The ordering provider generates the referral, ideally with diagnosis codes, clinical notes, and urgency level attached.
- Documentation transfer. Relevant records (labs, imaging, prior visit notes) are compiled and sent to the receiving provider before the appointment.
- Prior authorization. Insurance approval is obtained where required, before scheduling is confirmed.
- Scheduling. The patient is booked with the specialist or receiving provider, with confirmation sent to both patient and referring office.
- Patient confirmation and follow-up. The patient is reminded, confirmed, and followed up with if they miss or reschedule.
- Loop closure. The specialist sends a consult note or outcome summary back to the referring provider, completing the information cycle.
Where It Breaks
The Institute for Healthcare Improvement has documented that failures to close referral loops are patient safety risks, not just administrative inefficiencies. In practice, breakdowns cluster at predictable points:
- Missing or incomplete records at the time of transfer
- Prior authorization delays that push scheduling back by days or weeks
- No-contact with patients who don't respond to outreach
- Unclear ownership of follow-up between the referring and receiving teams
- No visibility into whether the appointment was actually kept
Each of these is solvable with the right process design. But solving them requires treating referral coordination as a workflow with defined ownership at every step, not a task that gets handled when someone has time.
What Referral Coordinators Actually Do
The referral coordinator is the person who owns the workflow described above, or as much of it as their organization has actually assigned to them. In most practices, that scope is broader than the job title suggests.
Core Responsibilities
- Receive and triage referral orders. Review incoming referral requests from providers, flag urgent cases, and confirm the referral contains enough information to move forward.
- Validate insurance and demographics. Confirm the patient's coverage is active, identify the correct specialist network, and catch eligibility issues before they cause downstream delays.
- Collect and transfer clinical records. Pull the relevant documentation from the EHR, request records from external providers if needed, and send a complete package to the receiving provider.
- Secure prior authorization. Submit auth requests to payers, track approval status, follow up on pending or denied requests, and document outcomes in the patient record.
- Route to the appropriate specialist. Match the referral to the right provider based on specialty, network status, patient location, and availability.
- Schedule the appointment. Book the visit, confirm with the patient, and coordinate timing with the receiving office.
- Document and track status. Keep referral status current in the EHR or referral management system so the ordering provider and care team have visibility.
- Follow up on no-shows and gaps. Contact patients who missed appointments, reschedule when appropriate, and flag cases where follow-through has stalled.
The Part That Doesn't Show Up in Job Descriptions
Beyond the task list, referral coordinators are doing relationship management work that rarely gets acknowledged. They are negotiating with payer representatives on authorization timelines, navigating specialist offices with varying intake processes, and managing patients who are confused, anxious, or disengaged from their own care.
Think of the role as part traffic controller, part patient advocate, and part operations backstop. When a referral falls apart (because records were missing, the auth was denied, or the patient never answered the phone) the coordinator is usually the person who catches it and tries to recover it.
That combination of administrative precision and human follow-through is what makes the role hard to automate entirely and easy to underestimate.
Why the Job Is Getting Harder
The referral coordinator role has always been demanding. What's changed is the volume, the fragmentation, and the accountability expectations, without a corresponding increase in the tools or support most coordinators actually have.
According to the American Medical Association, practices handle roughly 40 prior authorization requests per week. The IHI and NPSF nine-step referral framework has documented referral scheduling completion rates as low as 35%, meaning in many settings nearly two-thirds of referrals never result in a kept appointment.
More Volume, More Systems, Less Visibility
The core problem is structural. Referral coordinators are being asked to manage higher throughput across more disconnected systems than ever before:
- More referrals per coordinator. Patient volumes have increased and specialist capacity has tightened, which means more referrals to track and fewer easy scheduling options.
- More prior auth burden. Payer requirements have expanded. More procedures require authorization, timelines have lengthened, and denial rates have climbed.
- More portals. Coordinators are now logging into multiple payer portals, specialist EHRs, and referral management platforms, each with different workflows and status-tracking logic.
- Less standardization. Each specialist office has its own intake process, documentation requirements, and communication preferences. There is no universal protocol.
The Accountability Gap
What makes this particularly difficult is that referral coordinators are now accountable for outcomes they don't fully control. If a patient doesn't show up, the coordinator is expected to know why and to have tried to prevent it. If the specialist never received the records, the coordinator is expected to have confirmed delivery. If the auth was denied, the coordinator is expected to have appealed it.
IHI and MGMA-aligned frameworks both emphasize the same principle: every step in a referral workflow needs a clearly defined owner. "Write this down, publish it for the team, and ensure there is no step owned by nobody." In most practices, that clarity doesn't exist.
The result is a coordinator who is simultaneously a scheduler, an authorization specialist, a patient outreach agent, a records retrieval coordinator, and a status-tracker, often across a caseload of dozens of open referrals at any given time.
This is not a staffing problem that gets solved by hiring more coordinators. It is a process design and tooling problem. The coordinators doing this work are not failing, the systems around them are.
What Skills Do You Need to Be a Referral Coordinator?
Strong referral coordinators combine clinical knowledge, administrative precision, and communication skills that most job postings don't fully capture. Here are the ten that matter most in real workflows:
- Medical terminology. Understanding diagnosis codes, procedure codes, and clinical language is essential for reviewing referral orders, communicating with specialist offices, and documenting accurately.
- EHR proficiency. Most referral workflows run through an electronic health record. Coordinators need to navigate patient records, generate referral orders, attach documentation, and track status without friction.
- Prior authorization knowledge. Understanding which procedures require auth, how to submit requests to different payers, how to read denial reasons, and how to initiate appeals is now a core competency, not a specialty skill.
- Payer portal navigation. Each major insurer has its own portal with its own auth submission and status-tracking process. Coordinators who can move efficiently across multiple portals save their team significant time.
- HIPAA compliance. Handling patient records, communicating across provider organizations, and using third-party platforms all require consistent attention to privacy and data handling requirements.
- Documentation accuracy. Incomplete or inaccurate documentation is one of the most common reasons referrals stall. Coordinators need to be precise and thorough, especially when transferring records to outside providers.
- Patient communication. Reaching patients to confirm appointments, explain next steps, and follow up after missed visits requires clear, empathetic communication across phone, text, and portal channels.
- Follow-through and case ownership. The ability to track dozens of open referrals simultaneously, flag stalled cases proactively, and close loops without being prompted is what separates effective coordinators from reactive ones.
- Cross-team coordination. Referral coordinators work across billing, clinical, front desk, and external provider teams. Navigating those relationships without creating friction requires organizational awareness and communication judgment.
- Referral management tool fluency. Increasingly, practices use dedicated referral management or care coordination platforms alongside their EHR. Comfort with these tools (and the ability to learn new ones) is becoming a baseline expectation.
Do You Need a Degree to Be a Referral Coordinator?
No. Most referral coordinator positions do not require a four-year degree. Employers typically prioritize relevant administrative experience, medical office background, payer familiarity, and EHR comfort over formal education credentials.
What employers are actually looking for: experience in a healthcare administrative setting, demonstrated knowledge of insurance and authorization processes, and the ability to work in an EHR. A candidate who has spent two years in a medical front office handling scheduling and insurance verification is often a stronger hire than a recent graduate with a healthcare administration degree and no clinical environment experience.
That said, certifications do matter, both for job eligibility and for salary progression. The three most relevant pathways for referral coordinators are:
Certification Pathways
- CMAA (Certified Medical Administrative Assistant). Offered by the National Healthcareer Association (NHA). Requires a high school diploma or GED plus a short training program or relevant experience. This is the most accessible entry-level credential and the most commonly cited for referral coordinator roles. Best for candidates new to healthcare administration or looking to formalize their skills.
- CHAA (Certified Healthcare Access Associate). Offered by the National Association of Healthcare Access Management (NAHAM). Requires 6 to 12 months of patient access experience before sitting for the exam. Better suited for coordinators working in hospital registration environments or centralized referral centers where formalized patient access processes are standard.
- CHAM (Certified Healthcare Access Manager). Also through NAHAM. Designed for supervisory and leadership roles within healthcare access management. Appropriate for coordinators moving into team lead or referral operations manager positions.
Certifications signal competency to employers and can meaningfully affect starting salary and advancement potential. They are also achievable without a college degree, which makes the referral coordinator role one of the more accessible career paths in healthcare administration.
How Much Does a Referral Coordinator Make?
Salary data for referral coordinators varies meaningfully by source, market, and employer type. The national picture across major sources in 2026 looks like this:
- Hourly range: approximately $19.42 to $20.15 per hour nationally, depending on the source (Indeed, PayScale)
- Annual range: most sources cluster between $48,000 and $52,000 at the national median, with the U.S. Bureau of Labor Statistics and Zippia-style aggregators converging around $50,000
- High end: large health systems, hospital-based roles, and positions in high-cost metros can push total compensation to $60,000 or above
What actually moves the number: location is the single biggest factor, followed by care setting (hospital vs. ambulatory vs. FQHC), workflow complexity (whether the role includes prior auth or just scheduling), and whether the coordinator holds a relevant certification.
A coordinator managing a high-volume specialty referral queue with full prior authorization responsibility in a large health system is doing a materially different job than someone handling simple scheduling referrals in a small primary care office, and the compensation should reflect that, though it doesn't always.
The section below breaks this down by state. Florida is included specifically because it surfaces as a People Also Ask question on the "referral coordination" SERP, and the data there is worth addressing directly.
Referral Coordinator Salary by State (Including Florida)
The table below reflects synthesized 2026 salary estimates across major data sources (Indeed, Salary.com, Glassdoor, Talent.com, Zippia). Where sources diverge, the range reflects that spread rather than forcing a false single figure.
| State | Annual Range | Hourly Range | Notes |
|---|---|---|---|
| California | $54,000 to $62,000 | $26 to $30 | High COL metros drive the upper end |
| New York | $52,000 to $60,000 | $25 to $29 | NYC-area roles skew higher |
| Massachusetts | $51,000 to $58,000 | $25 to $28 | Strong health system demand |
| Washington | $50,000 to $57,000 | $24 to $27 | Seattle metro pulls averages up |
| Illinois | $48,000 to $54,000 | $23 to $26 | Chicago-area roles dominate |
| Texas | $44,000 to $50,000 | $21 to $24 | Wide range across metro vs. rural |
| Arizona | $43,000 to $49,000 | $21 to $24 | Phoenix-area growth driving demand |
| Ohio | $42,000 to $48,000 | $20 to $23 | Midwest average; varies by system size |
| Georgia | $42,000 to $48,000 | $20 to $23 | Atlanta health systems at the higher end |
| Florida | $42,000 to $46,000 | $18 to $22 | See note below |
Florida Salary Note
Florida referral coordinator salaries in 2026 cluster between approximately $42,000 and $46,000 annually based on data from Salary.com ($41,790), Talent.com ($42,224), and Glassdoor ($45,480). Indeed reports an hourly average of $18.33, which it notes is roughly 12% below the national average.
The spread across sources is meaningful: a coordinator at a large Florida health system (UF Health reports averages around $24.85/hr on Indeed) will earn significantly more than the state average suggests. Metro market, employer size, and whether the role carries prior authorization responsibility all affect actual compensation.
Methodology note: these figures are sourced from publicly available salary aggregators and should be treated as directional estimates. Actual compensation varies by employer, experience level, certifications held, and specific workflow scope.
What Strong Referral Coordination Looks Like Now
Given everything above (the workflow complexity, the prior auth burden, the completion rate data) what does a well-run referral coordination function actually look like in 2026?
The honest answer is that it looks less like a single coordinator heroically managing everything and more like a team with clear process design, defined ownership, and the right tooling supporting them.
The Before/After on Referral Coordination Maturity
| Reactive (common) | Proactive (best practice) |
|---|---|
| Referral status tracked in spreadsheets or EHR notes | Centralized referral tracking with real-time status visibility |
| Authorization submitted after scheduling is attempted | Auth initiated at referral creation, before scheduling |
| Patient follow-up happens when someone has time | Automated outreach triggers at defined intervals |
| Loop closure depends on specialist sending notes | Active follow-up protocol if consult note isn't received within X days |
| Ownership unclear between referring and receiving teams | Every step has a named owner and a documented handoff point |
| Dropped referrals discovered only when patients complain | Stalled referrals flagged proactively by status age |
What This Means for Practice Leaders
Strong referral coordinators are still the core of the function. The judgment calls (how to handle a complex auth denial, how to communicate with a patient who is resistant to follow-through, how to navigate a specialist office that isn't responding) require human expertise that no workflow design eliminates.
But the manual overhead of tracking, chasing, and documenting across disconnected systems is where coordinators lose the most time and where the most referrals fall apart. Practices that have closed the gap between reactive and proactive coordination have done it by giving their teams better visibility and reducing the amount of manual status-chasing required.
That's the role automation plays in this space: not replacing coordinator judgment, but handling the repetitive tracking and outreach work that currently crowds out the higher-value parts of the job. When coordinators spend less time chasing status updates, they spend more time on the cases that actually need their attention.
If your referral workflows are still running on manual tracking and reactive follow-up, the completion rate data above is a reasonable benchmark for what that's costing you.
FAQ: Referral Coordination Quick Answers
What does referral coordination mean?
Referral coordination is the end-to-end process of managing patient referrals between providers. It includes initiating the referral, transferring clinical documentation, obtaining prior authorization, scheduling the appointment, confirming patient follow-through, and closing the loop with outcome information. It is a defined operational function, not just an administrative task.
Do you need a degree to be a referral coordinator?
No. Most referral coordinator positions do not require a four-year degree. Employers typically look for relevant administrative or medical office experience, EHR familiarity, and insurance knowledge. The CMAA certification (offered by the NHA) is the most accessible credential for the role and requires only a high school diploma or GED.
What skills do you need to be a referral coordinator?
The core skills are medical terminology, EHR proficiency, prior authorization knowledge, payer portal navigation, HIPAA compliance, documentation accuracy, patient communication, follow-through and case ownership, cross-team coordination, and referral management tool fluency. The combination of administrative precision and communication skill is what separates effective coordinators from reactive ones.
How much does a referral coordinator make in Florida?
Florida referral coordinator salaries in 2026 cluster between approximately $42,000 and $46,000 annually, with an hourly range of roughly $18 to $22 depending on employer and market. Indeed reports a state average of $18.33 per hour, approximately 12% below the national average. Large health system roles and metro markets skew higher.

Sami scaled Simple Online Healthcare to $150M and built a multi-specialty telehealth clinic across 20 specialties and all 50 states. Connect on LinkedIn.
Sami Malik is the Founder and CEO of Linear Health, an AI-native healthcare operations platform that automates referral coordination for specialty clinics, primary care groups, and FQHCs. Before Linear Health, he scaled Simple Online Healthcare to $150 million and built a multi-specialty telehealth clinic across 20 specialties and all 50 states.
Connect with Sami on LinkedIn or learn more about inbound referral coordination and outbound referral coordination solutions.
Improve Your Referral Coordination Workflow
If you're evaluating how to reduce manual referral tracking and follow-up, see how Linear Health automates the closed-loop workflow end to end.