How Multi-Location Practices Use Voice AI to Scale Patient Access
There's a specific moment in the life of a growing specialty group when the phone system turns from a minor annoyance into an operational crisis. It usually happens around location four or five.
Loading audio...
There's a specific moment in the life of a growing specialty group when the phone system turns from a minor annoyance into an operational crisis. It usually happens around location four or five.
At two locations, you could manage. Your original front desk team knew every provider's quirks, every insurance panel, every weird scheduling rule. Then you opened a third site, hired new staff, and spent two months training them before they could answer a call without putting someone on hold. Then a key person quit. Then you acquired another practice with completely different workflows. Now your phones ring constantly, your hold times are climbing, and you're hemorrhaging referred patients who gave up waiting.
Sound familiar? You're not the only one. And here's the part nobody wants to hear: hiring more people won't fix this.
The math that breaks every multi-location group
The numbers are simple and painful. A 10-location specialty practice fields somewhere around 400 inbound calls a day across all sites. Even a 15% abandonment rate means 60 patients per day called your practice and hung up before anyone could help them. If a third of those patients call a competitor instead (and the data says they do), and the average patient lifetime value sits between $3,000 and $5,000, that's somewhere around $60,000 to $100,000 per day in potential revenue walking out the door.
You could hire more front desk staff. But healthcare front desk turnover runs 30% to 40% annually. A new hire takes four to eight weeks to get comfortable with your scheduling rules. So you're essentially training people as fast as you're losing them, and during every transition period, call quality drops and patients fall through the cracks.
The problem isn't your people. Your people are working their tails off. The problem is that the phone model doesn't scale. Every new provider, every new location, every new referral source adds call volume. Headcount grows linearly. The gap gets wider.
Why most voice AI breaks at multi-site scale
Here's something that isn't obvious until you've tried it: most AI voice agents for healthcare were designed for single locations. They can answer phones for one office with one set of scheduling rules and one provider roster. That works fine for a two-doctor clinic.
But you're not running a two-doctor clinic. You need the AI to route calls to the right location. You need it to know that Location A has different insurance panels than Location B. You need it to understand that Dr. Kim only sees patients on Tuesdays at the Northside office but Thursdays at Main. And you need all of that information in a single dashboard where your operations team can see the full picture without logging into five different systems.
When you deploy a single-location tool across multiple sites, you end up managing multiple instances of the same product. Separate configurations. Separate reporting. Separate headaches. That's not automation. That's just multiplying the original problem.
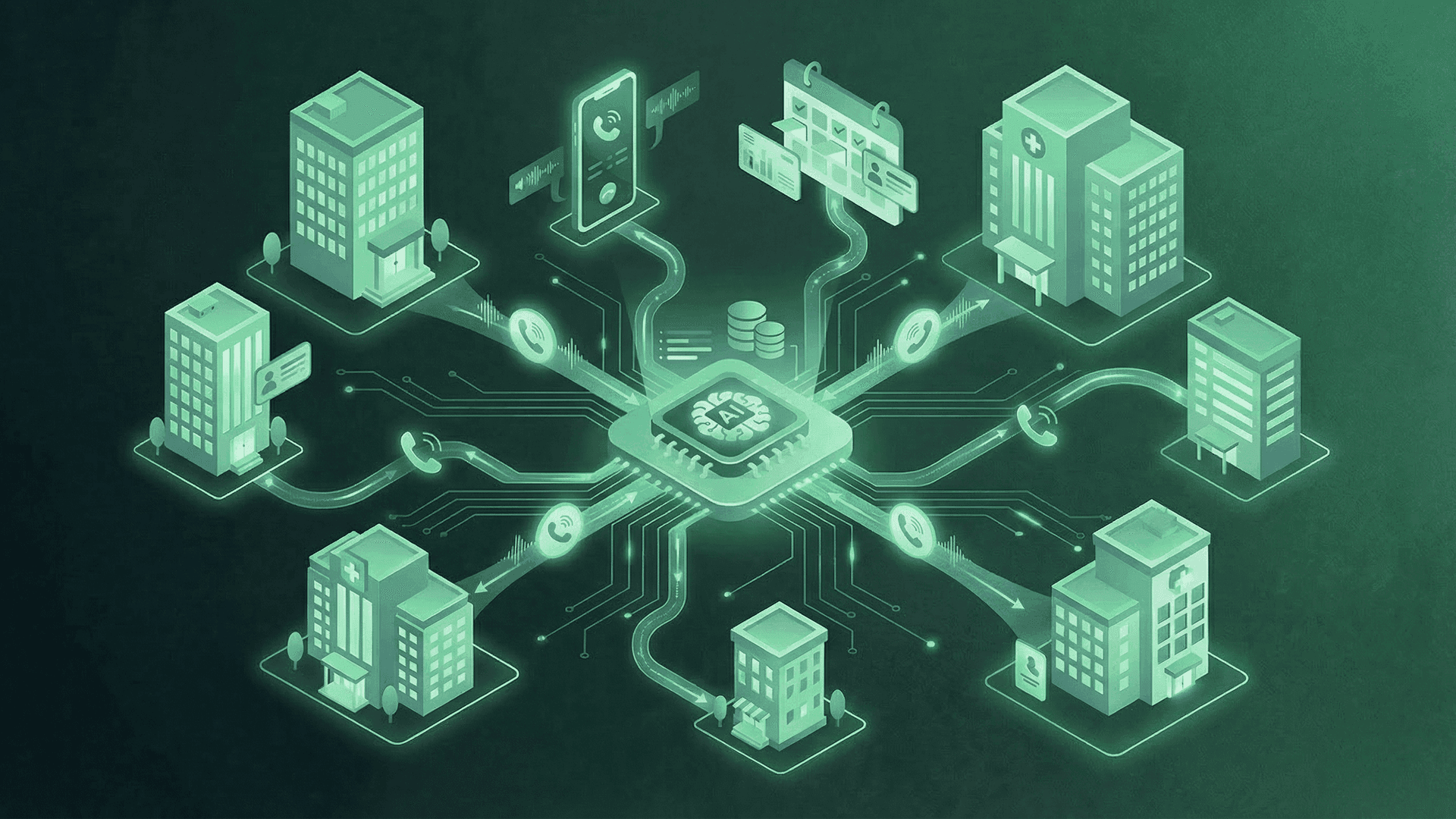
What connected voice AI looks like at scale
The architecture that works for multi-location groups is centralized configuration with per-location customization. One platform manages your entire practice network. Each site has its own scheduling rules, provider roster, and insurance panels, but it's all configured in one place.
When a patient calls, the AI figures out which location they need (from the number they dialed, their patient record, or simply by asking) and applies the right scheduling logic for that site. If Location A doesn't have availability for what the patient needs, the AI can offer Location B fifteen minutes away without transferring the call or asking the patient to call a different number.
The reporting piece is just as important. Centralized analytics with per-location drill-down means your operations leaders see call volume, resolution rates, no-show metrics, and scheduling performance across every location in one dashboard. When hold times spike at your Westside office, you see it in real time instead of hearing about it from an angry physician three weeks later.
And the patient experience gets consistent. Every person who calls any of your locations gets the same quality of interaction. No more "the Eastside office is great but good luck getting through to Midtown." The AI doesn't have bad days, doesn't call in sick, and doesn't need three months of training before it can handle a complex scheduling call.
Managing phones across multiple locations?
Linear Health provides centralized voice AI with per-location customization, unified reporting, and 85%+ call resolution. Go live in 4 weeks per site.
The PE playbook for portfolio deployment
For PE-backed healthcare groups, the phone problem compounds with every acquisition. Each new practice comes with its own phone system, its own front desk habits, its own scheduling idiosyncrasies. Standardizing operations post-acquisition is one of the hardest parts of integration, and the front desk usually gets addressed last because leadership sees it as a people problem rather than a systems problem.
It's a systems problem.
PE-backed healthcare groups deploying voice AI across portfolio acquisitions can standardize operations in weeks rather than months. The playbook works like this:
Weeks 1-2: Assess the acquired practice. Map their call volume, scheduling rules, EHR setup, and front desk workflow. Configure the AI with location-specific rules.
Weeks 3-4: Go live. The AI handles scheduling, rescheduling, cancellations, and general inquiries. Existing staff keep handling the complex stuff while the AI absorbs the volume.
Month 2: Measure. Resolution rates, patient satisfaction, staff time recovered. Fine-tune the call flows based on what the data says, not what anyone guesses.
Month 3 onward: The acquired practice runs on the same platform as the rest of the portfolio. Same reporting structure. Same operational baseline. Same patient experience.
Compare that to hiring and training a new front desk team from scratch (two months to get them proficient, with a coin flip on whether they stick around past year one) and manually stitching together operational data from separate systems for your quarterly board deck.
Before and after: what the numbers look like
Let's put this in concrete terms. A 10-location orthopedic and pain management group, 35 providers.
Before:
- 400 inbound calls per day across all sites
- Hold times averaging 4 to 6 minutes
- Abandonment rate at 18%, meaning 72 patients per day who called and gave up
- 22 front desk staff
- Referred patients waiting 3 to 5 business days for first contact
- No-show rate running at 22%
After deploying connected voice AI:
- Same 400 calls per day
- Hold time drops to zero because the AI picks up instantly
- Abandonment falls below 3%
- The AI resolves 85% of calls without staff involvement
- Referred patients get contacted in under 5 minutes
- No-show rate drops to 13%, a 40% reduction from automated multi-channel reminders
- Same 22 staff members, now spending their time on patients in the building instead of patients on the phone
Nobody got fired. The job just got better. Turnover drops because front desk work becomes less soul-crushing. Patient satisfaction climbs because hold times disappear. Referring physicians send more patients because they see faster loop closure.
That's not a technology transformation. It's an operations transformation that happens to use technology.
Getting started without boiling the ocean
You don't need a big-bang rollout. Start with your highest-volume location or the one with the worst phone metrics. Configure the AI for appointment scheduling (your highest-volume, most measurable call type). Run it for 30 days. Look at resolution rates, abandonment rates, and staff feedback.
If the data looks good (and it will), expand to the next two locations. Then the next three. Within 90 days you can have your entire network running on a single connected platform with centralized reporting and 3:1 ROI within weeks of each site going live.
The question isn't whether voice AI works for multi-location specialty practices. That's settled. The question is how much longer you can afford to run your phones the way you're running them now.
Frequently Asked Questions
Can voice AI handle different scheduling rules at each location?
Yes. Connected voice AI supports centralized configuration with per-location customization. Each site maintains its own provider roster, scheduling rules, insurance panels, and call routing logic, all managed from a single platform with centralized analytics.
How do PE-backed groups typically deploy voice AI across portfolio practices?
The most effective approach is staged deployment: configure for one acquired practice (2 to 4 weeks), go live, measure for 30 days, then expand. This is significantly faster than hiring and training new front desk staff at each acquisition, and delivers 3:1 ROI within weeks per site.
What metrics should we track for a multi-location voice AI deployment?
The key metrics are call resolution rate (target 85%+), average hold time (target zero), call abandonment rate (target under 5%), no-show rate change, and staff time recovered per location. Centralized analytics with per-location drill-down is essential for multi-site operations.
Does voice AI replace front desk staff?
No. Voice AI handles the repetitive 40% of front desk work: scheduling calls, rescheduling, general questions, prescription refill requests. Staff time shifts to complex patient needs, in-person interactions, and exception handling. Most practices maintain the same headcount but see improved satisfaction and lower turnover.

Sami scaled Simple Online Healthcare to $150M and built a multi-specialty telehealth clinic across 20 specialties and all 50 states. Connect on LinkedIn.